Rotator Cuff Tears
Sports Medicine and Physical Therapy Services for Rotator Cuff Tears.
What Are Rotator Cuff Tears?
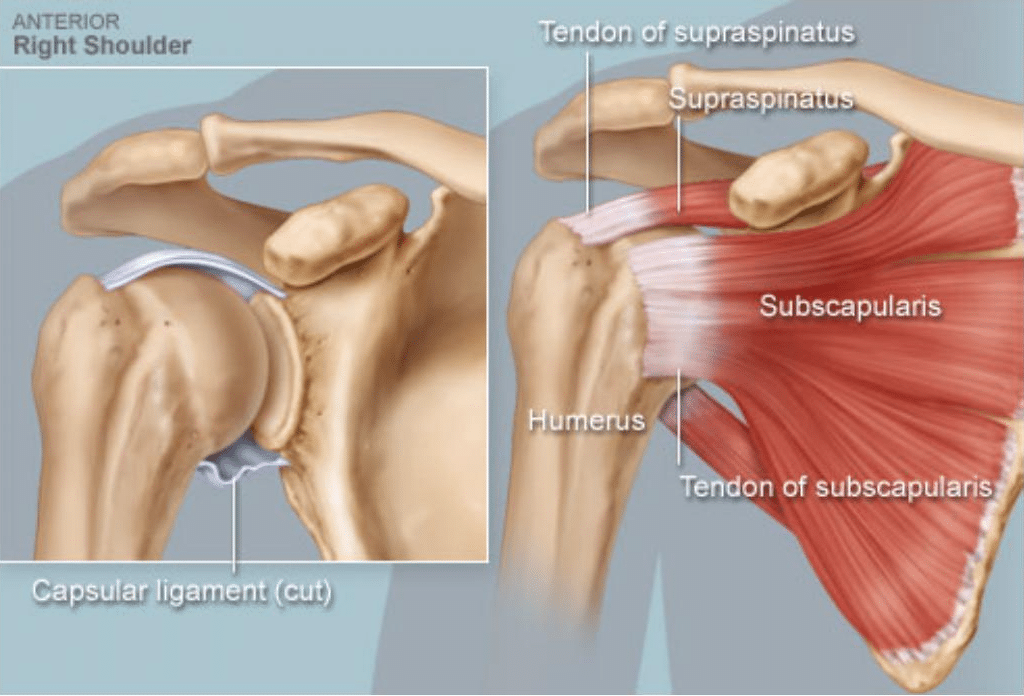
How Do I Tear My Rotator Cuff?
Some tears are traumatic, from a specific injury event, while others are degenerative, created by wear and tear over the years. A common mechanism for traumatic tears is falling on your outstretched arm or elbow. Dislocations of the shoulder joint, in those usually older than 40, can tear the cuff. Cuff tears can also occur from lifting something heavy with a jerking motion.
Are There Different Types of Tears and What are Symptoms of Each Type?
The most common distinction of tear types is partial thickness or full thickness tears.
- Partial thickness tears damage the tendon but does not completely sever it from the bone. These tears are often quite painful. When the muscle contracts it pulls on the remaining connection to the bone. Sometimes these tears are small enough that they are difficult to notice weakness. In general, tears greater than >50% of the thickness of the attachment to bone will not heal on their own, and may go on to a full thickness tear.
- Full thickness tears completely separates the tendon from the bone, creating a hole. These tears may or may not be painful. The tear usually results in noticeable weakness. Weakness may be in external rotation (infraspinatus and supraspinatus tears), interval rotation (subscapularis tear), and holding your arm away from your body at shoulder level (supraspinatus). These tears do not heal on their own. They may retract (pull away) from the area of attachment, and scar down. Over time the muscle tissue will atrophy and eventually be replaced by fat (fatty infiltration) which may make it difficult or impossible to repair with good function.
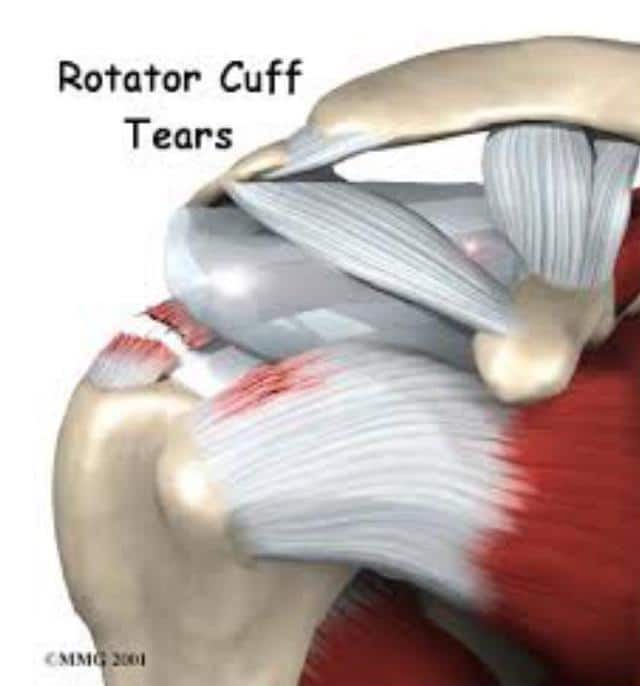
How Are Rotator Cuff Tears Diagnosed?
Most rotator cuff tears can be diagnosed by obtaining a good history of the injury event or long term overuse of the arm, and a thorough physical exam focused on passive and active range of motion, strength of the shoulder muscles, and inspection for atrophy of the cuff muscles. Large tears are easier to pick up on exams than small tears. Pain, however, can cause the patient to appear weak on examination of cuff muscles even if there is not a tear. An injection of numbing medication into the space above the rotator cuff, in combination with re-testing strength, may help distinguish if the weakness is just from pain or from tendon injury.

Do I Need Imaging Studies?
- X-rays are routinely obtained to be sure there is not a fracture (avulsion of bone attached to the tendon), calcification in the tendon, or other abnormalities including a bone cyst or tumor. The rotator cuff is a “soft tissue” and is not visible on an X-ray. There may be other clues that a cuff has been torn for some time. Without an intact rotator cuff, the humerus may move up in the joint towards the acromion, and the glenohumeral joint may develop signs of arthritis (joint space narrowing, bone spurs, etc…)
- Ultrasound may be performed in the office to evaluate the cuff tissues. An ultrasound is very good at picking up inflammation or calcification in the cuff tissue, and a well trained physician can accurately identify both partial thickness and full thickness tears. It is harder to tell if the muscle tissue is atrophied or has fatty infiltration. It can also be harder to evaluate a rotator cuff that has previously undergone repair.
- MRI or MR Arthrogram may be used to get a good overall picture of the soft tissues and bone in the entire shoulder area. It can accurately diagnose inflammation of the tissues, partial and full thickness rotator cuff tears, and measure retraction of the tendon, muscle atrophy and fatty infiltration. It may also find other causes of symptoms including labral tears or cartilage injury.
If I Have a Rotator Cuff Tear, Do I Need Surgery?
Not all rotator cuff tears require repair. Many older individuals go about their daily lives unaware of having a tear.
- If a partial tear is causing symptoms that are not alleviated by at least 6 weeks of physical therapy and injections, a repair may be recommended. Platelet rich plasma (PRP) injection may enhance healing in a partial tear.
- A large tear causing weakness in a younger or more active patient should be fixed as soon as range of motion has been regained to avoid retraction of the tendon, atrophy and fatty infiltration of the muscle and arthritic changes in the joint.
- An older individual with a full thickness tear, but low demands on the shoulder, may be effectively treated with cortisone injections and a home exercises program.
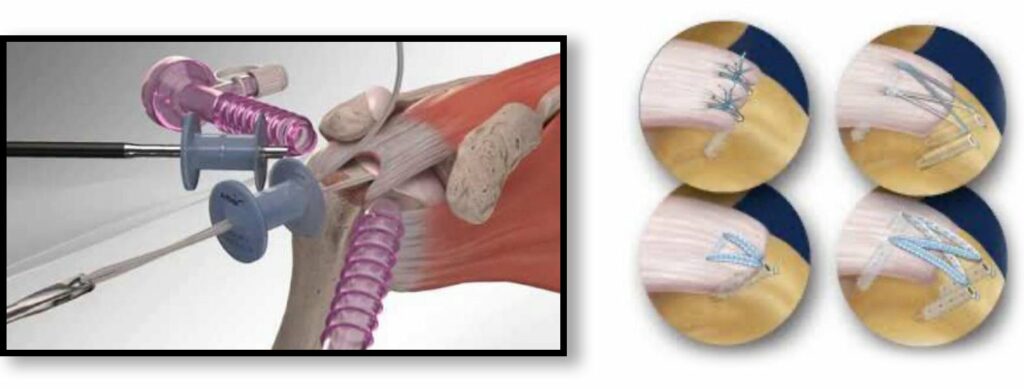
If I Choose Surgery, What Does That Mean?
Historically, rotator cuff repairs were performed through large incisions to expose the tendons and overnight hospital stays. Today, with the aid of the arthroscope, most surgeries are performed in the outpatient setting with patients going home the same day. The arthroscope allows excellent visualization of the rotator cuff from its underside within the joint (articular side) and from above in the subacromial space (bursal side) and allows for placement of repair devices through small plastic cannulas. This is performed through 3 or 4 small incisions (portals). The cuff is repaired using small anchors in the bone with the attached sutures passed through the cuff tendon. Suturing the tendon to the bone seals the tear from the joint fluid and the compression of the tendon on the bone encourages healing of the tendon to the bone. If the tissue quality is less reliable or the tear pattern is complex, after the initial arthroscopy it may be helpful to expand one of the small incisions into a slightly larger one, splitting but not cutting any muscle fibers (“mini-open” technique), to perform a reliable repair.

How Long Is The Recovery After Surgery?
During the first 3-6 weeks, the shoulder is immobilized (sling with a large pad holding the arm out) to protect the repair and allow the swelling and pain to decrease. It also helps you learn to avoid using your arm for lifting, pushing or pulling. You can do simple pendulum exercises and move the elbow to avoid stiffness. Physical therapy is then started to begin working on range of motion and wake up the muscles around the joint.
A tendon takes about 10-12 weeks to heal to the bone. By three months, most repairs are “healed” but the cuff muscles are weak, as they should not be stressed with exercises in the early healing phase. It will take another 2 months or more of rotator cuff and scapular stabilization exercises to regain enough strength to use the shoulder normally or return to overhead activities or sports.