Knee Replacement (Total Knee Arthroplasty)
Sports Medicine and Physical Therapy Services for Knee Replacements.
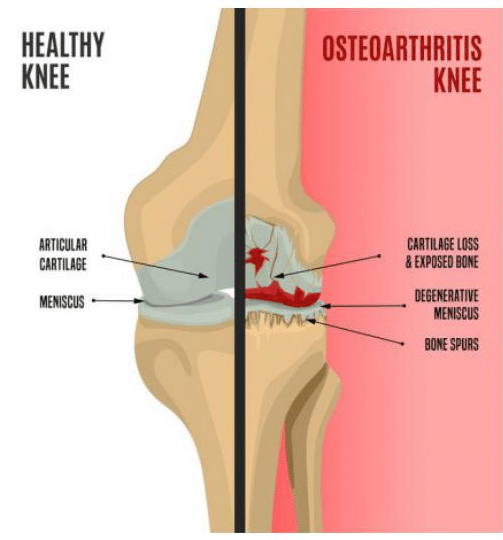
Who Needs a Knee Replacement?
Should I Consider Knee Replacement Surgery?
You may want to consider knee replacement surgery if you have:
- X-ray Findings Of Joint Space Narrowing
- Osteophytes (Bone Spurs)
- Leg Alignment Changes (Bow Legged or Knock-kneed)
- Persistent Joint Swelling
- Decreased Range Of Motion
There are many conservative treatment options. Consider joint replacement if you have failed:
- Activity modifications to avoid high impact activities
- Exercises to strengthen the muscles that cross the joint and improve range of motion
- Anti-inflammatory or non-narcotic pain medications, oral or topical
- Joint injections (cortisone, platelet rich plasma (PRP), viscosupplementation)
- Compression sleeve or unloader brace
- Arthroscopic surgery to address mechanical symptoms or repair injured tissue
Most knee replacements are performed on patients between 50-80 years old. If you can wait until you are in your 60’s or 70’s, there is a good chance the surgery will last your lifetime. However, there is no “magic age” to have a replacement. Some people do not feel they can wait any longer, due to loss of quality of life, and may proceed at a younger age, understanding they may require a revision surgery in the future. The decision to proceed should be made after in-depth discussions with your surgeon and a thorough understanding of the procedure and its risks.

What Does it Actually Mean to Have a Knee Replacement?
A TKA (total knee arthroplasty) and a TKR (total knee replacement) are the same thing. In a “total,” all the worn cartilage surfaces are removed with a saw (about one centimeter thick cuts) and similar thickness metal implants are used to cap the remaining bone. There are high quality plastic liners that separate the metal implants. You keep many aspects of your native knee including the joint capsule tissue, quadriceps tendon, patellar tendon and patella, the medial and lateral collateral ligaments and often the posterior cruciate ligament. The remaining meniscus and the anterior cruciate ligament (ACL) are removed, but the knee is stabilized by other functions of the implant. The cartilage surface of the patella may be left alone or resurfaced with a plastic implant depending on the individual situation. Once the procedure is performed you cannot go back to your native knee, as key tissues have been removed.
How Long is Recovery From a Knee Replacement?
The most critical period of recovery occurs during the first 3 months, when you are working hard to decrease pain and swelling, improve range of motion and wake up the muscles around the knee using physical therapy, home exercises and often a stationary bicycle.
Most people are able to return to work within a month, if their job does not require them to stand all day or lift, push or pull heavy objects. The majority of patients continue to take over the counter medications (Tylenol and anti -inflammatories) and ice daily for several months. Some patients are able to return to activities such as light hiking after just a few months.
There will be days and nights during those first few months that you will wish you had not had the surgery, but in the end, most people comment they wonder why they waited so long. You may continue to see improvements for 1-2 years after surgery as you regain overall strength and endurance.
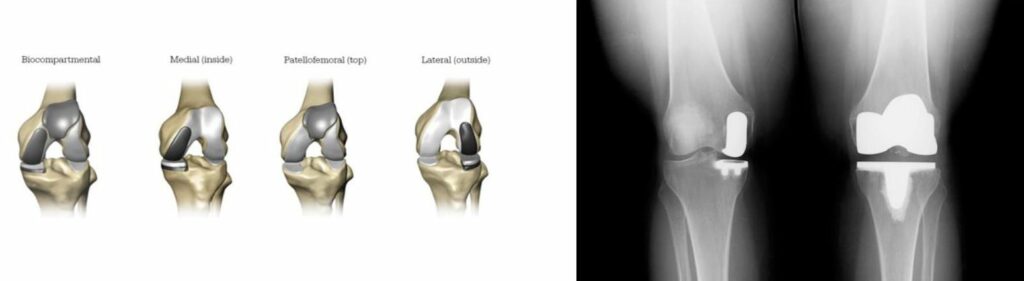
Can I Have a Partial Knee Replacement Instead of a Total?
There are three compartments in the knee: medial, lateral and patellofemoral. Each compartment can be replaced independently of the others (Unicompartmental knee replacement), but ONLY IF the other compartments are not showing any signs of cartilage wear or contributing to your pain, and the alignment and range of motion are near normal.
Replacing one compartment may not prevent progression of arthritis in the other two compartments, and a partial knee replacement may have to be revised (a second major surgery removing the old implants and placing new implants) to a total knee replacement down the road. If a partial replacement is done in an appropriate patient it may last more than a decade. Partial knee replacement may be a good option for a younger patient with post-traumatic arthritis in one compartment or an older patient with osteoarthritis wear in only one compartment. It may “feel” more like your natural joint, as the ligaments in the center of your knee are retained. These surgeries may be done with the assistance of a robot. Our surgeons are trained to use the MAKO robotic knee replacement system, as well as the standard technique using cutting jigs.
What are the Risks and Benefits of Total Knee Replacement?
The main goal is to improve your quality of life. Joint replacement surgery is a safe and effective procedure to relieve pain, correct leg deformity, regain range of motion, and help you resume normal daily activities. Many people are able to return to pain-free sleep, walking, hiking, biking, water sports, skiing, golf and doubles tennis, among other activities.
Are There Any Serious Risks Involved With Joint Replacement?
As with any surgery, there are risks. In general, if you are healthy and active the risks are LOW ( <2%)
You should discuss your overall health with your primary care provider (PCP) prior to planning surgery. Your PCP can estimate and discuss your relative risk associated with a major surgery, and may want to perform further tests before granting you “clearance” for surgery.
Specific risks associated with the knee during and after surgery include:
- Infection (2%)
Infection can occur soon after surgery or even many years later. Oral antibiotics are used prior to dental procedures to help avoid late infections. Treatment may require multiple surgeries and a long course of IV antibiotics to clear the infection. On very rare occasions, infections do not go away despite treatment and could lead to amputation. - Arthrofibrosis (Stiffness)
Participating in Physical Therapy and home exercises may help prevent this problem. If you remain stiff, a manipulation under anesthesia to improve the knee’s ability to bend may be recommended. It is important to get the leg straight early on to avoid a permanent loss of extension. There are no good treatments for this problem and it may affect the way you walk, leading to hip and back pain or arthritis. - Extensor mechanism disruption (patella fracture, quadriceps tendon rupture, patellar tendon rupture)
These complications are usually associated with a fall after surgery. Most are repairable allowing the knee to actively straighten again. If not, however, the knee will not function well as may need to be braced, fused or amputated to regain function. - Deep venous thrombosis (DVT or blood clot) (<4%) and pulmonary embolism (rare)
Blood thinners such as Aspirin, Xeralto, Eliquis , Warfarin or Lovenox may be prescribed immediately after surgery to help prevent or treat a blood clot. Clots that go unrecognized or untreated can break off and go to the lungs which can be life-threatening. Early mobilization helps decrease the risk of a DVT. - Persistent Pain or Swelling
These symptoms may continue despite a well performed knee replacement. Medications and time may lessen the symptoms. - Injury to Nerves, Arteries, or Veins
Major injuries are very rare. In severe valgus deformity knees (knock-kneed), there is a higher chance or nerve pain or even a foot drop. A nerve on the outside of the knee shortens in length as the deformity progresses and may be stretched as the knee alignment is restored. This usually responds to nerve medications and gets better with time. Most patients have skin numbness on the outside of the knee for some time, as a sensory (feeling only) nerve must be cut to gain access to the knee for replacement. It does not affect muscle activity. - Loosening of the Implant, Mechanical Failure or Long-term Wear
Recent studies show about 90% of knee replacements remain functional at 15 years. It is recommended that you avoid participating in high impact activities such as running or sports that require jumping or pivoting quickly, as that may disrupt the connection between your bone and the surgical implant. BMI (body mass index) of >40 has been associated with higher failure rates, so staying fit is important. Loose or worn out implants may need revision surgery.