Kneecap Pain (Patellofemoral Pain Syndrome)
Sports Medicine and Physical Therapy Services for Kneecap Pain.
What is Patellofemoral Pain Syndrome?
What Area of the Knee is Affected?
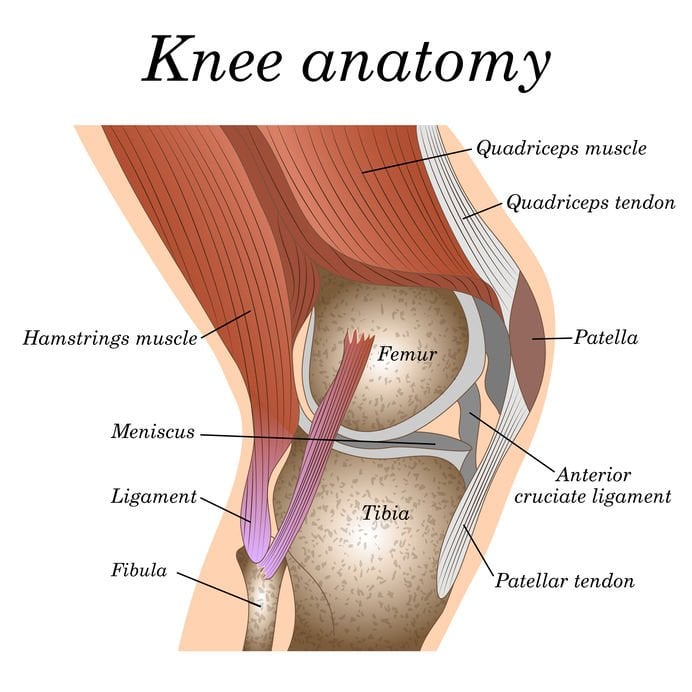
The knee is a large hinge joint comprised of the femur (thigh bone), tibia (shin bone), and patella (kneecap). The muscles in the front of the thigh, the quadriceps act to extend or straighten the knee. The hamstrings in the back of the thigh act to flex or bend the knee (and extend the hip). The patella sits in a groove in the femur (trochlear groove). The quadriceps tendon attaches to the patella and the patella links the quadriceps tendon to the patella tendon which inserts into the tibia. From a biomechanics standpoint, the patella acts as an anatomic pulley for the quadriceps and increases the lever arm of the extensor mechanism allowing the quadriceps to function more effectively to extend the knee.
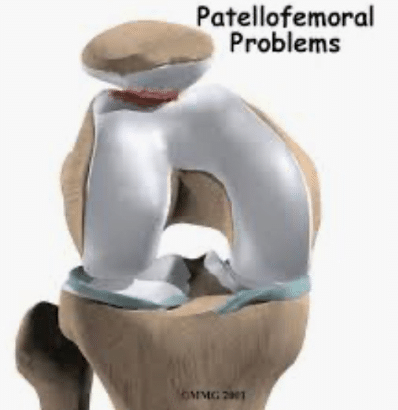
Articular cartilage lines the under the surface of the patella and the surface of the trochlear groove. Normally, the cartilage is quite thick, with a smooth surface and quite dense. Chondromalacia is a term given to the condition when the articular cartilage starts to soften and develop fissures.
What Does the Exam Entail?
After discussing your history (including sports/fitness activities and prior injuries), your doctor will examine the knee. Measures of quadriceps muscle tone and joint swelling are noted. A patella compression test can measure patella pain when the quadriceps contract and pull on the patella. Also, checking for crepitus (rough feeling) as the knee is extended and flexed can provide information about articular cartilage break down.
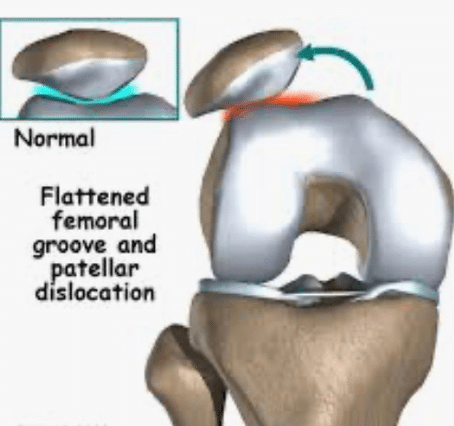
X-rays may be taken to look at the alignment of the patella in the trochlear groove (and look for other possible injuries in the joint that might create similar symptoms). The patella should track in the middle of the groove. With PF pain syndrome the patella often tracks laterally to the outer edge of the trochlear groove.
An MRI could provide information about the condition of the articular cartilage. But the treatment plan would not be altered even with this information, so the MRI is not warranted initially.
What are the Causes of PF Pain Syndrome?
Several factors can add up to create this injury. Primary suspects are quadricep weakness and malalignment during activities that cause the patella to track to the lateral side of the trochlear groove.
Weak Muscles
Weakness in the quadriceps may allow the patella to not track correctly in the trochlear groove. If even a trace amount of swelling is present, the inside quadriceps muscle (vastus medialis) is inhibited and the other quadriceps will pull the patella laterally. Do not participate in PF pain-producing activities if the knee is swollen. We typically see this when athletes are returning from ACL or meniscus surgery.
Weak hip muscles (hip abductors and external rotators) do not maintain proper hip/knee/foot alignment and allow the knee to fall into a valgus position. Simply put, the patella will track in a plane between the hip and the foot. If the knee falls into valgus, the patella will track laterally.
Tight Muscles
- Tight hamstrings and quadriceps can increase loads on the patella as the knee extends when running.
- Tight ITB (Iliotibial Band) can pull the patella laterally.
- Tight Achilles (especially in the soleus muscle) can cause excessive pronation in the foot during the support phase in the running cycle. The excessive pronation can cause the patella to track laterally. In addition, the tight Achilles tendon can force people to run with the foot everted to the outside. Again, since the patella tracks in a plane between the foot and hips, if the foot is everted to the outside, the patella will track laterally.
Training Errors (for Runners):
- Increasing running mileage too quickly.
- Running too many days per week.
- Shoes may be broken down or not provide adequate support.

What is the Treatment?
- Strengthen quadriceps, hips, and hamstrings with a combination of single-joint isolation exercises and multi-joint exercises. Follow the guidelines discussed in “PF strength exercises”. Work on flexibility of the hamstrings, IT Band, hips, quadriceps, and Achilles.
- Modify training to allow adequate recovery between training sessions. If your shoes are worn out or do not provide adequate support, replace them. New shoes are cheaper than x-rays. Over the counter shoe inserts that provide more arch support may help decrease pronation. Runners may benefit from changing running mechanics to more of a mid-foot strike rather than a heel-strike and increasing stride rate can help reduce shock loads on the patella.
- Conservative, non-surgical treatment is usually successful in treating PF pain syndrome. If the knee swells and remains swollen for more than a week, damage to the articular cartilage may have occurred. If conservative treatment fails and the knee continues to swell, injections with corticosteroids may be beneficial. Other types of injections can be discussed with your doctor.
If conservative options are not successful, then surgical treatment may be indicated. Your doctor can discuss options with you.