Lateral Collateral Ligament (LCL) Injuries
Sports Medicine and Physical Therapy Services for Lateral Collateral Ligament (LCL) injuries.
What is an LCL?
What are the Symptoms of an LCL Injury?
Pain can be felt along the outside part of the knee – from just above the joint line (where the femur and tibia meet) to just below the joint line. Typically, the knee is swollen over the site of the injury. The knee may feel unstable when trying to walk. In addition to the ligament’s stability being compromised, the pain and swelling also inhibits the quadriceps from helping provide support.

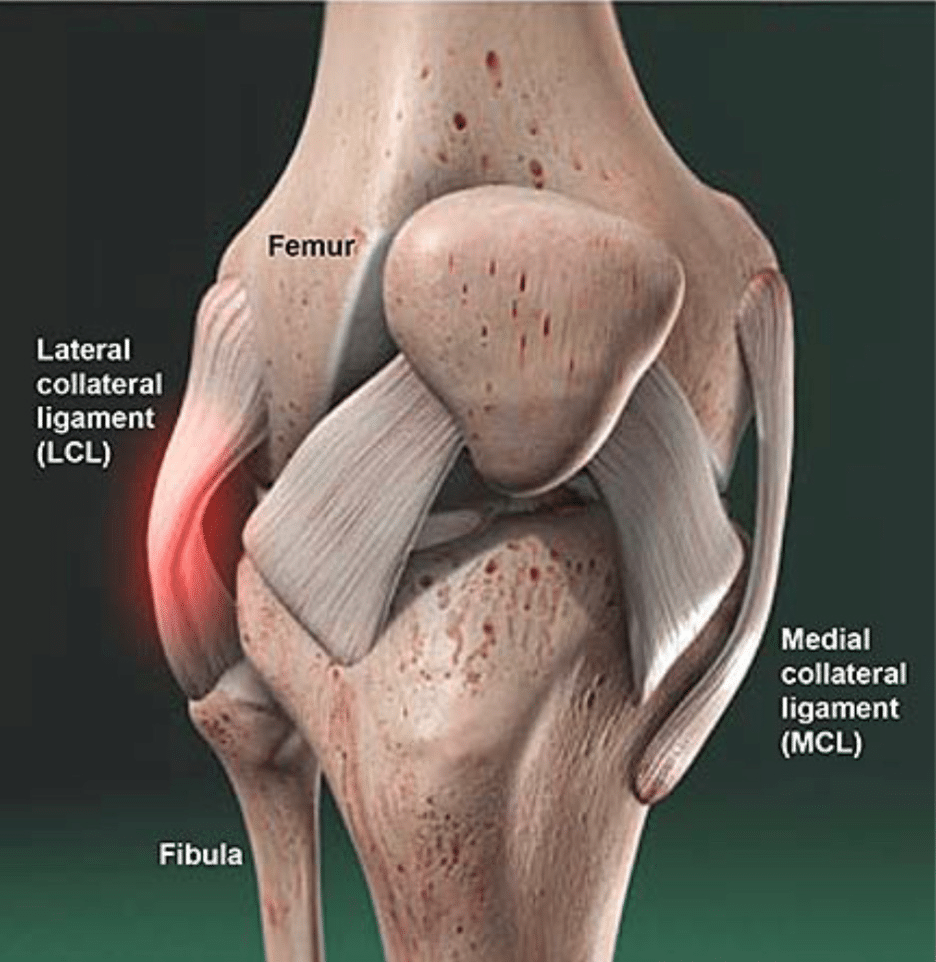
How Do You Tear the LCL?
Injuries to the LCL are usually caused by a direct blow to the inside/front of the knee that pushes the knee outward. The MCL can be injured by a blow to the outside of the knee. LCL injuries are not as common as MCL injuries.
How is the Diagnosis Made?
The most accurate way to make a diagnosis is through a good history. The patient can often describe the injury producing situation – foot was planted and got hit on the inside/front of the knee. If the knee were struck just slightly more anterior (in front), then often the posterior cruciate ligament is injured instead or in addition to the LCL. The doctor’s examination of the knee includes checking for areas of pain and gently testing the side to side stability of the joint. Forward and backward translation are also examined to check stability of the cruciate ligaments. More forceful injuries may also damage the posterolateral corner of the knee (popliteus muscle tendon, popliteofibular ligament, and other stabilizers in the back corner of the lateral knee). If the posterolateral corner is injured the knee will exhibit increased external rotation when stressed. More severe tears can cause numbness or weakness in the foot. This happens because the peroneal nerve is near the LCL and may be stretched at the time of injury or compressed by swelling of the surrounding tissues.
Injured ligaments are considered “sprains” and are graded on a severity scale.
- Grade 1 Sprains. The ligament is mildly damaged; it has been stretched slightly but still provides stability to the knee.
- Grade 2 Sprains. The ligament is partially torn; stability is compromised but there is still an endpoint when the knee is lightly stressed with a manual test.
- Grade 3 Sprains. The ligament is completely torn, and joint rotational stability is further reduced. This level of injury often involves the posterolateral complex in the knee and may require surgery.
Are X-Rays and MRI Needed?
X-rays will not show the injury to the MCL (or other ligaments or cartilage) but can show whether the injury also caused a fracture in a bone.
MRI scans can provide images of the ligaments and other soft tissues. The information from the MRI may not change how the LCL is treated, but information about other structures (cruciate ligaments, meniscus, and posterolateral corner) may affect treatment plans.
What is the Treatment for LCL Injuries?
Injuries to the LCL usually respond well to non-surgical treatment. A hinged brace will be used to protect the ligament from sideways forces and allow the ligament to heal. It is important that a brace be utilized as soon as possible to help achieve the best possible outcomes from the injury. Rehabilitation exercises (basic isometric exercises and resistance training exercises) should be initiated soon after the injury. Based on the severity of the injury, and individual recovery, your doctor will recommend that the brace be worn at all times initially and then gradually decrease the use of the brace. For example, the brace may be prescribed full-time for the first 6 weeks and then worn during workouts and during sports for 3 months. Your doctor will give you a specific timeline based on your injury and your progress. Surgery may be necessary if the posterolateral corner has significant damage and rotational stability is compromised.
When Can I Return to Sports?
A progression needs to be followed to limit the chance of re-injury or sustaining a different injury. Strength needs to be restored with resistance exercises. The brace will be worn during the return to sports phase and worn once back playing sports. Once the athlete can walk without a limp, straight ahead running can begin. If the athlete can run without a limp, then agility drills and sport drills can be started. Once these drills can be performed without a limp or favoring the knee, the athlete can return to sports.
If surgery is necessary, the return to sports will be delayed to allow adequate recovery time for repairs to heal and then more time is required to rehabilitate the knee.